Shoulder joints can become painful and difficult to move. Often this lack of movement is caused by the joint surfaces not moving smoothly on each other or by tendons and ligaments tightening (contracting) around the joint.
The joint may be too painful to move. Joint replacement can help ease these symptoms. The operations (sometimes called arthroplasty) replace the surfaces of the joint, which are normally made of bone covered with cartilage, with parts made of metal and plastic.
Do I need a shoulder joint replacement?
You may need a joint replacement if:
- your pain can’t be eased enough by other methods, such as drugs, injections or physiotherapy, and is affecting your quality of life
- you can’t use your arm easily
- you have a bone fracture close to the joint that can’t be fixed
Joint replacement surgery should be considered carefully in consultation with your surgeon who will be able to advise you on what the surgery involves and on the pros and cons of having or delaying an operation.
What are the possible advantages of shoulder or elbow joint replacement surgery?
In most cases you can expect that your joint pain will disappear or be much reduced once the wound has healed. Because the joint will be less painful, you’ll probably notice that your range of movement increases. However, this may take several months of hard work and may not happen at all for some people.
Shoulder and elbow joint replacements are very successful and most people are delighted with the results and the improvement to their quality of life.
What are the possible disadvantages of shoulder or elbow joint replacement surgery?
A replacement joint can never be as good as a natural joint and extreme movements such as hanging washing or reaching for high shelves are often not possible, although most people will be able to carry on with simple everyday activities.
You should discuss with your surgeon before an operation how much they expect your movement to improve, as each case is slightly different.
Replacement joints will also wear out after a time, but it’s likely that they’ll last for 10 years.
What are the alternatives to joint replacement surgery?
Most people with arthritis of the shoulder will receive other treatments from either their GP, physiotherapist or a rheumatologist before they see a surgeon for a joint replacement. These may include:
- drug treatments, including painkillers and non-steroidal anti-inflammatory drugs (NSAIDs)
- disease-modifying anti-rheumatic drugs (DMARDs) if you have rheumatoid arthritis
- injections of steroid and other drugs into the joint
- injections of local anaesthetic to numb nerves
- physiotherapy
If these treatments don’t improve the pain, you may need surgery.
In some cases, other operations are more helpful than joint replacement, such as:
- cleaning out the joint (debridement) to ease pain
- removal of the lining of the joint (synovectomy) if it’s very inflamed (this isn’t usually carried out on the shoulder joint)
- removal of part of the bone (the radial head) at the elbow
What are the different types of shoulder joint replacement?
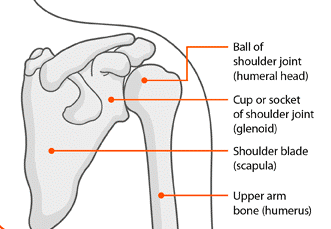
The shoulder is a ball-and-socket joint. The end of the upper arm bone (the humeral head) forms the ball, while part of the shoulder blade (the glenoid) forms the socket.
Shoulder replacement surgery replaces the ball and sometimes the socket with man-made parts. There are several types of shoulder replacement surgery:
Hemiarthroplasty is where the ball part of the joint (the humeral head) is replaced with an artificial ball component with a stem that extends into the shaft part of the bone. This is usually used for fractures but is also used in many cases of arthritis.
Shoulder resurfacing is a different type of hemiarthroplasty where, instead of removing the humeral head and replacing it with an artificial ball on a stem, a metal cap is fitted over the ball part of the joint. This means less bone has to be removed during the operation.
Total arthroplasty is where both the ball (of the upper arm) and socket (of the shoulder blade) are replaced. This is increasingly used for very specific kinds of arthritis depending on your age, how badly worn the natural joint is and the state of the tendons around the joint. Occasionally a total arthroplasty will be carried out using a resurfacing component.
Reverse anatomy arthroplasty is where the artificial components are fitted in reverse – that is, the socket to the upper arm bone and the ball to the shoulder blade. Currently this is only used in patients with severe arthritis of the shoulder joint and very poor tendon cover around the joint. It can sometimes be used if a patient has both a severe joint fracture and poor tendon function.
Your surgeon will consider which type of joint replacement will be most suitable for your shoulder problem. They’ll discuss this and the possible complications with you, and you’ll then have time to think things through before you decide whether to go ahead.
The operation will be carried out using a general anaesthetic (in which case you’ll be asleep) and/or a local anaesthetic (which numbs the nerves to the arm and shoulder). The shoulder joint is normally opened from the front or top and the muscles moved out of the way (retracted). The damaged bone of the humeral head is then removed and the remaining bone is prepared for the artificial component to be fitted.
