Transurethral resection of a bladder tumour (TURBT) is a procedure used to cut away any abnormal growths (tumours) that may have developed in your bladder. Any growths are then tested to see if they are cancerous and if they are, how advanced the cancer is. If the tumour is on the lining of your bladder and hasn’t grown down into the surrounding muscle (non-muscle invasive), TURBT can be an effective treatment.
There are other tests for bladder cancer, but TURBT is the recommended procedure to both diagnose and treat it.
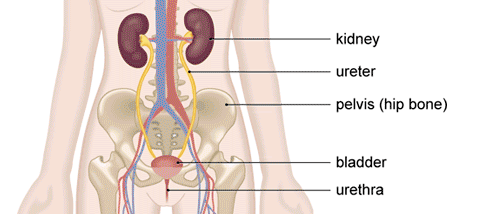
This form of cancerous growth starts in the bladder lining. Some of the symptoms associated with the condition are listed below:
- Bladder tumours can bleed, resulting in your urine containing blood (haematuria).
- Blood clots can sometimes form, resulting in your bladder being unable to empty efficiently.
- Burning sensation apparent when passing urine.
- Feeling the need to pass urine more frequently.
If your surgeon has recommended a trans-urethral resection of a bladder tumour (or TURBT), be aware that the choice is yours as to whether you wish to go ahead with the procedure. The contents of this page will inform you of the benefits and risks associated with the procedure, and therefore enable you make an informed decision. However, if you have questions that are not addressed in this paper, check with the surgeon, or your healthcare team.
What are the types of bladder tumour?
Invasive – these are cancers that grow into and through the wall of the bladder. The cancer can also spread to other areas of the body.
Non-invasive – these mainly stay within the bladder lining. It is the most common type of bladder cancer. There is a risk of the development of an invasive tumour from a non-invasive one (between 10 and 15 in 100).
The tissue removed by the surgeon is examined under a microscope in order to determine the type of tumour that you have. You might have just the one tumour, but there is also a chance you may have a number of them. The surgeon can also perform a biopsy (the removal of small pieces of tissue) on the parts of your bladder that appear to be unaffected. From these they can determine if the cells that make up the bladder lining are becoming unstable, and therefore have an increased likelihood of forming tumours (known as carcinoma in situ).
What benefits are there?
The symptoms should get better. By scraping away (resecting) a non-invasive bladder tumour, it should completely remove it and there will be a reduction in the risk of the development of an invasive cancer. If the cancer is invasive, a TURBT will not get rid of the cancer entirely. Examining the tissue under a microscope however, will enable the surgeon the recommend the best type of treatment for your case.
What are the alternatives to surgery?
Resection of the tumour is the only dependable way to determine what sort of tumour you have.
What happens if I decide against having the operation?
With a superficial tumour, the risk will be that it will turn into a cancerous one. With a cancerous tumour, the risk will be that it will grow deeper into your bladder tissue and the cancer might then spread to other parts of the body.
Procedure
Depending on the size and how many tumours you have, the operation can take between 15 and 40 minutes.
During the procedure your surgeon passes a cystoscope (a thin, tube-like telescope) along your urethra (the tube that passes urine out of your body). They will then feed this up into your bladder. A camera lens at the end of the cystoscope sends pictures from the inside of your bladder to a monitor. This allows your surgeon to see any unusual growths on your bladder wall. Your surgeon then passes a wire loop along the side of the cystoscope. This loop has a safe electrical current passing through it, which creates heat. Using this, your surgeon guides the tumour away from your bladder wall and in the process, seals the area to stop any bleeding.
Your surgeon will also remove some deeper tissue. Sometimes, cancerous lumps can grow outwards or into the muscle layer of your bladder (muscle invasive bladder cancer). This is less common than the non-muscle invasive type, but testing the deeper tissue can confirm whether or not this has happened.
Any growths or samples of bladder tissue that are removed during the procedure are sent to the laboratory for testing.
Your surgeon then takes the cystoscope out and passes a thin, flexible tube (catheter) into your urethra. Your catheter will allow you to pass urine. It’s also used to flush your bladder through after the procedure and give you the chemotherapy medicine mitomycin C. It will normally be left in place during your stay in hospital.
Are they any other forms of treatment needed?
Even if you may not have an invasive cancer, it may be that your surgeon recommends a single dose of chemotherapy, going straight into the bladder via the catheter. This is known as intravesical chemotherapy, and given this way, the chemotherapy can reduce the risk of any new growths developing in the bladder lining.
In order to help the operation be successful:
- If you are a smoker, stop smoking immediately. Smoking is a key contributing factor to the development of this form of cancer. Stopping now reduces the potential for new bladder tumours developing. Quitting smoking several weeks before the procedure will help to reduce the risk of developing complications, as well as improving your health in the future.
- You increase your risk of developing complications when you are overweight. If possible, try to maintain a healthy weight.
- Exercising regularly will aid preparation for the procedure, as well as recovery from it. Check with your GP before undertaking an exercise regime.
How long does it take to recover?
Whilst in the hospital
When the operation has finished, you will get transferred first to a recovery area, and then on to a ward. After one to two days the catheter will be be removed, and you should be able to return home once you have passed urine. it could be that your consultant recommends that you remain a little while longer.
Once at home
Ensure you carefully follow the instructions given to you by the healthcare team in order to reduce the risk of a blood clot. This may mean that you have been given medication, or are required to wear special stockings.
It could be that you will encounter a stinging sensation the few couple of times that you pass urine. Ensure that you drink plenty of water, as not only will it reduce the risk of blood clots, but it will also make it easier for you to pass urine. You should be able to return to work after two weeks. In the first week, it is not recommended that you do strenuous exercise. It is not unusual to experience blood in the urine whilst any raw areas are healing in the the bladder. If it gets full and painful, make sure to contact your consultant, as it may be that you have a blood clot. If this is the case, you might be required to return to hospital to remove it using a catheter. Exercising regularly is recommended in order to recover as soon as possible. Before beginning an exercise regime, check with your consultant. Do not drive, unless you are confident that you have complete control over your vehicle. It is vital to check this with your doctor.
In future
Results from your operation will be discussed with you by your consultant, although biopsy results will not be available for a few days. It could be that you are required to return to the clinic for these results.
Non-invasive tumour – you will be required to have regular cystoscopies (from 1-6 weeks to annually), to see if any new tumours have developed.
Invasive tumour – the treatment options will be discussed with you by your surgeon.
If you have carcinoma in situ, the surgeon may recommend an intravesical chemotherapy course. This should help reduce the risk of any new tumours developing.
