If you have an overactive thyroid (hyperthyroidism), it means your thyroid gland is making too much thyroid hormone.
Too much thyroid hormone speeds up your body’s metabolism. Your metabolism is the combination of chemical processes that happen in your body, such as those that change the food you eat into energy. When your metabolism speeds up, you may lose weight even though you’re eating more, and have other symptoms such as a fast heart rate.
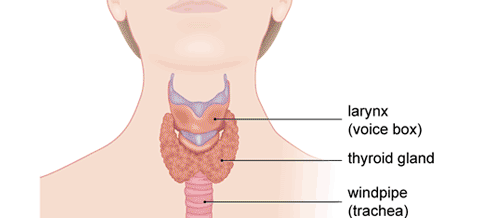
Your thyroid gland is in your neck, in front of your windpipe. It produces two hormones called thyroxine (T4) and triiodothyronine (T3).
Symptoms of overactive thyroid
If you have an overactive thyroid, the symptoms can vary from mild to severe. Symptoms can also be different depending on your age, and can sometimes seem like an existing health problem has got worse.
How severe your symptoms are doesn’t always reflect how severe your condition is. For example, you may have mild symptoms but have a severely overactive thyroid. The symptoms you have can also depend on what’s causing your overactive thyroid.
The main symptoms of overactive thyroid include:
- feeling hot / less able to cope with heat
- losing (or sometimes gaining) weight
- feeling hungry and eating more
- feeling tired with weak muscles
- sweating more than usual
- having irregular or no periods
- feeling emotionally up and down, restless and irritable
- having a lump in your throat (this is called a goitre and can be caused by a large thyroid gland)
- feeling nervous and anxious
- shaking (tremors)
- a fast or irregular heart rate
Diagnosis of overactive thyroid
Your GP will ask about your symptoms and examine you. They may ask you about your medical history, and if anyone in your family has an overactive thyroid gland.
If your GP thinks you may have an overactive thyroid, they will ask you to have one or more blood tests. This is to check the level of thyroid hormones in your body. The main hormones measured in blood tests are:
- TSH – thyroid stimulating hormone
- FT4 – free T4 (the active part of thyroxine)
- FT3 – free T3 (the active part of triiodothyronine)
If you have an overactive thyroid, you will have a low TSH level with a high FT4 level and a high FT3 level. The exact levels of hormones measured may vary between different laboratories. So what’s classed as a normal, high or low level for each of the hormones may vary from one area to the next.
If the results of the blood tests show you have an overactive thyroid, your GP will refer you to a specialist. This will be an endocrinologist, who specialises in treating thyroid conditions.
A small number of people may also have a radionucleotide thyroid scan. This involves having a small amount of a radioactive substance injected into your blood. This can be seen inside your thyroid gland using a special camera.
Treatment of overactive thyroid
Treatment for overactive thyroid depends on what has caused it and how severe your symptoms are. Any treatment you have aims to lower your thyroid hormones levels and ease your symptoms.
Medicines
When you’re first diagnosed as having an overactive thyroid, your doctor may prescribe beta-blockers. These help to ease symptoms such as a fast heartbeat (palpitations) or shaking. You may need to take these until your thyroid hormone levels come down. If you can’t take a beta blocker, you may be given a medicine called a calcium channel blocker.
Your doctor may prescribe the antithyroid drugs, carbimazole or propylthiouracil. These help to reduce the amount of hormone your thyroid gland produces. These medicines usually work quite quickly, but it can take two to three weeks until you get the full benefit.
You’ll be asked to take these medicines for 12 to 18 months. You may be able to stop taking them, although up to half of people find that their symptoms come back after stopping treatment. If this happens, you may need to carry on with your medication, or try a different treatment.
If you’re pregnant, your doctor may change your medicines after the first trimester (the first three months). This is to make sure your baby develops properly and is healthy.
Radioiodine treatment
Radioactive iodine aims to destroy your thyroid gland, so that it stops producing hormones. You take radioactive iodine as a single capsule or tablet. It takes around three to four months to work fully.
Your doctor might suggest radioiodine treatment if:
- you can’t take the medicines for overactive thyroid
- you have other health conditions
- medicines for thyroid disease haven’t worked
Once the radioactive iodine has worked, your body won’t produce any more thyroid hormones. This means you’ll need to take levothyroxine (thyroid hormone replacement) for the rest of your life.
You can’t have radioactive iodine treatment if you’re pregnant or breastfeeding. You should also use contraception for at least six months after your treatment.
Surgery
Another option for treating an overactive thyroid is to have all or most of your thyroid gland removed. It’s not commonly used as a treatment. But your doctor may suggest it if:
- medicines and radioactive iodine treatments haven’t worked, or you can’t take them
- you need treatment very quickly
- you’re pregnant, or want to become pregnant in the next six months
After the operation, your body won’t produce any more thyroid hormones. This means you’ll need to take tablets for the rest of your life to replace them.
Monitoring your thyroid levels
During and after treatment for an overactive thyroid, you may need to have regular blood tests and check-ups. This is to measure the amount of thyroid hormones in your body and to check that treatment has worked. How often you will need these will depend on what caused your condition and what treatment you had. Your doctor will tell you what you need to do.
Causes of overactive thyroid
There are a number of causes of overactive thyroid. The most common cause is Graves’ disease, which is an autoimmune disease. This means that your body starts attacking your thyroid gland and it responds by producing too much hormone. Other causes of an overactive thyroid include:
- conditions which produce swellings on your thyroid gland
- some medicines, such as amiodarone and lithium
Complications of overactive thyroid
Most people with an overactive thyroid recover well after treatment. But some people may develop complications, some of which can be serious or life-threatening. The main complications are listed below.
- Heart problems, such as heart failure or an irregular and fast heartbeat (atrial fibrillation).
- Sight problems – if you have Graves’ disease, you may develop a condition called thyroid eye disease. Find out more about this by reading the FAQ Thyroid eye disease.
- Thyroid storm – this is a severe condition that needs emergency treatment. The symptoms include a high fever, heart problems and restlessness.
- If you’re pregnant, an overactive thyroid can mean your baby may be born early or underweight. It can also lead to miscarriage.
After treatment for overactive thyroid
While your thyroid was producing too much hormone, you may have felt hungry and eaten more to keep your weight up. After your treatment, you may need to eat less to avoid putting on weight.
Because treatment lowers the levels of thyroid hormone in your body, it’s important to make sure that these don’t become too low. If your hormone levels become too low, this is called hypothyroidism. The main symptoms are:
- putting on weight
- feeling the cold
- dry skin and hair
- lack of energy
- a puffy face
